What Doctors Don’t Tell You About Acute Hepatic Porphyria
Written by |

Editor’s note: This column was updated Sept. 15, 2020, to emphasize the individuality of the writer’s personal experience, and now specifies the importance of seeking guidance from medical professionals.
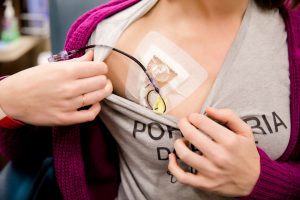
When my second port was implanted on the left side of my chest, just above my heart, I decided to give it a name. I dubbed it “Blake Lively,” because without its help in delivering my magical healing infusion treatment, it would be deadly. (The naming credit goes to my dearest friend, Jennifer.)
I receive infusions of heme frequently, often multiple times in a single week, and the medication is notoriously hard on ports. I’ve met several people with acute hepatic porphyria (AHP) who receive treatments as often as I do, and are on their fourth or fifth port. Those I’ve met were not told by doctors to expect a treatment plan like this when we received our hepatic porphyria diagnosis.
I’ve lived with an active case of AHP for more than 20 years, and I’ve learned from dozens in the porphyria community. Seeking care from medical professionals is necessary to porphyria care, but so is realizing that each patient case is unique. I’m certainly no medical professional and can speak only to my personal experience, but it’s clear to me that there’s a disconnect between what is clinically understood about AHP and what I have lived — specifically in the areas of chronic symptoms, the definition of an attack, and symptom frequency.
Chronic symptoms
My acute attacks are the pits, but my chronic symptoms are what truly interfere with my daily life. Discomfort such as shoulder stiffness, neck soreness, frequent headaches, and weakness and neuropathy in my hands affect my activities in varying and unpredictable degrees from day-to-day.
Little is widely understood about the pain people with porphyria experience between attacks. It’s challenging to discuss solutions to chronic pain, neuropathy, and fatigue with a medical team more focused on my acute episodes.
Definition of an attack
By the time I was diagnosed, I was in some sort of baseline attack nearly all the time. It wasn’t until I began receiving treatment that the fog started to lift and I was able to pinpoint my flares versus attacks, and cobble together a definition.
For instance, I can be curled up in pain in a fetal position for 24 hours, but the commonly understood definition of an attack is that it lasts a minimum of three days. In this case, my day of agony is a flare.
Additionally, some sources indicate that attacks typically don’t last longer than two weeks, but that’s not a rule I adhere to, as it’s a dangerous expectation to give my body. I’ve had multiple attacks — at least once a year during the previous four years — last over a month.
Frequency of symptoms
When I received my diagnosis, no one told me I could expect two attacks per month, coinciding with my monthly cycle. In fact, I was told I may have one, maybe two, annually. In my experience, giving a patient this expectation can be damaging.
For the first year or two of my porphyria journey, I pushed my body into all kinds of unhealthy situations (here’s an example of a business I started), with the understanding that with treatment, I would be a one-attack-per-year gal.
The discrepancies between lived experience and textbook knowledge used to be a source of immense frustration as I tried to understand what a life with porphyria meant. Plus, I certainly wanted to be better understood by medical professionals.
More importantly, my heart goes out to others with undiagnosed and diagnosed rare diseases who are looking for answers not always reflected in medical texts. Not having an expectation for what life looks like long-term is crazy-making, it requires learning to live in the moment, a certain acceptance of chaos, and finding joy in uncertainty.
Meeting and interacting with people who also have lived a porphyria experience supplements my medical care. The key is to find a group of people with a similar mindset who are choosing to move forward in their diagnoses, because it’s easy to get stuck in the suck when I’m in pain.
For anyone nodding their head right now who feels this frustration, and who struggles with embracing their chronic illness, I also recommend looking into medical research studies. I’ve had the privilege of participating in a natural history study on living with porphyria, and it has given me the opportunity to contribute to our society’s new and evolving understanding of what it means to live with chronic symptoms.
Not only is it satisfying to know that my experience may help others, it also is validating to think that in reporting my day-to-day challenges between attacks, my voice is finally being heard.
***
Note: Porphyria News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Porphyria News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to porphyria.



holly bucciarelli
Hi Claire.It's Holly Bucciarelli.I really liked this column.I've been in a "baseline"attack since March.It's 2:30 in the morning and I'm in too much porphyria pain that I can't sleep.When I lie down my diaphragm doesn't contract because of partial paralysis and causes severe chest pain and problems breathing.I'll start vomiting because of the pressure on my stomach.My daughter'so 17 years old and I've missed her whole childhood.This article shows the daily struggles.Thank you for writing it.We need someone with a voice and I don't think anyone is going to listen to me before it's too late.
Claire Richmond
Hi Holly! I'm so very sorry for your pain, your discomfort, the sheer exhaustion you must be in. That is such a long time to be experiencing a flare up of symptoms (not "intermittent" at all, right?), and while I wish I could do more to comfort you, it makes me smile to know that you can at least relate to my words. I can only imagine how you feel in regards to missing your daughter's childhood, this is so real and heartbreaking, I don't think enough people understand what it's like. My heart goes out to you and your family and I am humbled by your comments and readership. Thank you!
Darlene Maynor
I have just been diagnosed and no one has really told me anything except there's not much known and yes i have alot more health problems. Just found out and a little scared!!!!!
Claire Richmond
Hi Darlene! I'm so glad you reached out and that it sounds like you're getting some answers. You will get through this, but it will take some time to learn what you can expect for your body. Please keep relying on the community, it will help in times you feel most alone. Hugs to you!